Beyond the Quick Fix: A Modern Guide to Managing Low Back Pain
Low back pain is the leading cause of disability worldwide. It’s an almost universal human experience, yet it remains one of the most widely mistreated conditions in all of healthcare.
Despite record-breaking spending on treatments, results aren't getting any better. Why? Because we are constantly spoon-fed "quick fixes" and outdated advice—both on social media and in clinics that prioritize their bottom line over patient outcomes.
At Movement Spine & Sport, we’re adamant about staying on top of the latest research to change this narrative, continually striving to close the gap between what's always been done and what modern evidence actually suggests to be effective. If you’re currently navigating a low back pain flare-up, here are my top five strategies for a smarter, faster recovery.
1. Try Not to Panic
I know—easier said than done when your back feels like it’s on fire. But here is the most important thing to remember: Pain does not indicate tissue damage.
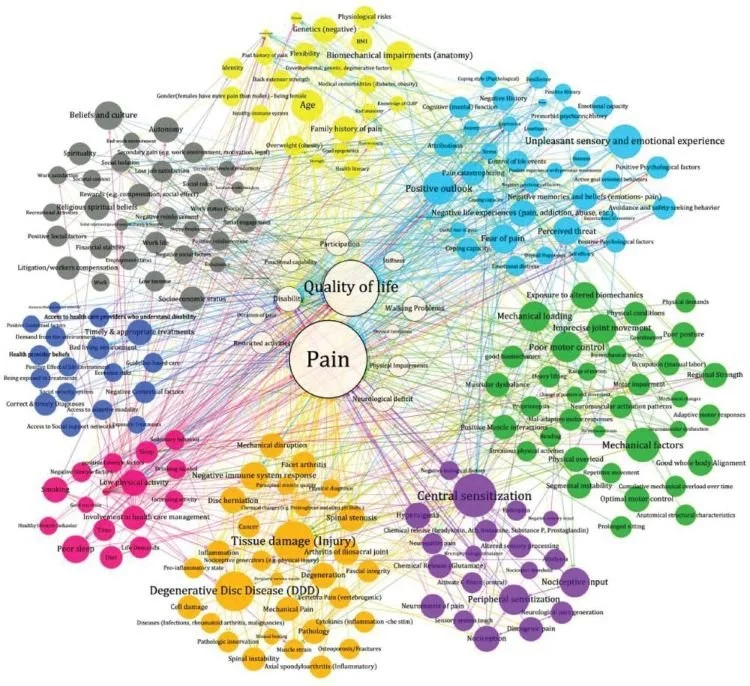
Pain is an individualized, multifactorial experience, not a death sentence. By refusing to let fear take over and viewing pain through a biopsychosocial lens, we can mitigate many of the unhelpful beliefs and false expectations that often stall recovery. Your body is adaptable and resilient; this episode will not last forever.
2. Keep Moving
Cliche as it may sound, movement is medicine. Whether it’s a brief walk, bodyweight exercises, or modified resistance training, getting blood flow to the area is critical.
The goal is to remain active safely. If a specific movement or exercise hurts, don’t stop moving entirely—just adjust factors such as the load, volume, tempo, or range of motion. Staying engaged in your training and day-to-day activities provides a massive boost both physically and mentally.
3. Stop Playing Detective
When attempting to overcome pain, it can be tempting to spend hours on Google or ChatGPT trying to find the exact tissue or joint that is "out of place." Don’t do it. Pain is multifactorial—it involves your nervous system, your stress levels, your sleep, and your movement patterns. You don't need to be a detective to get better. Identifying one specific structure as the "culprit" is often impossible and, frankly, unnecessary for a successful recovery.
4. Ignore the "Magic Exercise" Posts
This is my biggest pet peeve. Those "Top 5 Exercises for Low Back Pain" posts on Instagram lack the one thing you need most: context. Though they may be well-intentioned, the person posting them doesn't know your injury and training history, your pain triggers, or your goals.
Instead of hunting for a "magic" exercise, focus on:
Finding variations of the movements you enjoy that are currently pain-free
Supporting recovery via adequate sleep, quality nutrition, and stress management
Slowly reintroducing the provocative movements to show your brain that they are safe
5. Find a Competent Clinician
You don’t have to navigate this journey alone. Finding the right guide can make all the difference. A competent clinician should:
Listen to your entire story without making you feel rushed
Rule out any clinical red flags or medically serious pathologies
Empower you with ongoing education and a custom treatment plan
Encourage you to stay active rather than telling you to “just rest”
A good provider doesn't just treat you; they give you the tools and strategies to help you self-manage for the long run.
The Bottom Line
Maintaining a positive relationship with movement is the most effective tool in your arsenal for overcoming low back pain.
Moreover, recovery is seldom a straight line—sometimes we see substantial progress in as little as a few weeks, while other times it’s a longer process filled with ups and downs—but it is always possible.
Have questions about a recent flare-up or want to dive deeper into your personalized recovery plan?
Click here to get in touch with one of our team members—we’re here to help you get back to moving with confidence.
Ryan Lesik, D.C., CSCS
Movement Spine and Sport